Best Breathing Techniques for Anxiety and Dizziness
Experiencing dizziness, anxiety, or brain fog can make even the simplest daily activities feel overwhelming. Many of the patients I meet at California Brain & Spine Center in Calabasas describe moments when their mind feels clouded, their breath becomes shallow, and their balance feels unstable—all at the same time.
I’m Dr. Alireza Chizari, and in this guide, I will walk you through a powerful question many people ask: Can specific breathing exercises truly reduce dizziness, calm anxiety, and clear brain fog?
The answer is yes—when the exercises are done correctly and tailored to how the brain and autonomic nervous system actually function.
My goal is to help you understand why breathing affects the brain so deeply, and how to use step-by-step breathing techniques to stabilize your nervous system, restore clarity, and improve balance.
Why Breathing Affects Dizziness, Anxiety, and Brain Fog
Breathing is one of the fastest ways to influence the autonomic nervous system—the system that controls heart rate, blood pressure, vestibular reflexes, and mental clarity.
When breathing becomes:
- too fast
- too shallow
- irregular
…the brain receives mixed signals about oxygen, carbon dioxide, and bodily safety. This can lead to:
- dizziness
- increased anxiety
- difficulty concentrating
- brain fog
- lightheadedness
- a sense of internal “instability”
Breathing exercises work because they reset the balance between the sympathetic (fight-or-flight) system and the parasympathetic (rest-and-recover) system, helping your brain return to a stable baseline.
“Your breath is the remote control of your nervous system—learning to use it changes everything.”
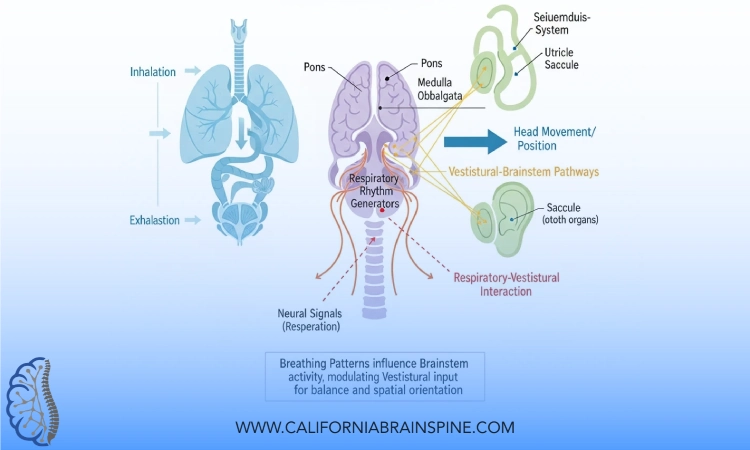
The Science Behind Breathing and the Brain
Breathing influences several brain networks involved in balance and cognition:
- Brainstem autonomic centers that regulate heart rate and vestibular responses
- Prefrontal cortex, which supports attention and mental clarity
- Insular cortex, which helps the brain interpret internal sensations
- Vestibular nuclei, which coordinate balance and spatial orientation
At California Brain & Spine Center, we see daily how proper breathing improves:
- dizziness from autonomic dysregulation
- anxiety-related vertigo
- post-concussion brain fog
- dysautonomia symptoms
- sensory overload
Breathing is not just relaxation—it is neurological rehabilitation when done with precision.
“When you change your breathing, you change your brain’s chemistry, rhythm, and ability to process the world.”
Step-by-Step Breathing Exercises for Dizziness, Anxiety, and Brain Fog

1. The 4-6 Regulating Breath
This is the fastest way to calm the autonomic system.
How to do it:
- Inhale through the nose for 4 seconds
- Exhale slowly for 6 seconds
- Repeat for 2–3 minutes
The longer exhale activates the parasympathetic nervous system, reducing:
- dizziness
- heart racing
- internal tension
2. Diaphragmatic Breathing to Restore Oxygen-CO2 Balance
This technique helps prevent dizziness caused by over-breathing.
Steps:
- Place one hand on the chest, one on the abdomen
- Slowly inhale into the lower hand
- Keep the upper hand as still as possible
- Exhale with relaxed lips
Repeat 6–8 cycles.
This restores healthy CO2 levels, reducing:
- lightheadedness
- stress-induced unsteadiness
- foggy thinking
“The diaphragm is the foundation of calm. When it moves well, the brain works better.”
3. Box Breathing for Mental Clarity
Excellent for brain fog and cognitive fatigue.
Technique:
- Inhale 4 seconds
- Hold 4 seconds
- Exhale 4 seconds
- Rest 4 seconds
This creates rhythmic stability between breath, heart rate, and neural processing.
Image note: “Therapist demonstrating box breathing on a whiteboard for a patient with dizziness and brain fog symptoms.”
4. Vestibular-Calming Breath with Head Positioning
Designed specifically for patients with dizziness.
Instructions:
- Sit upright with head neutral
- Inhale for 3 seconds
- Exhale for 6 seconds
- After 4 breaths, gently turn the head 5 degrees left
- After 4 breaths, gently turn 5 degrees right
This stabilizes the vestibulo-autonomic connection.
“Small head movements combined with slow breathing help retrain the brain’s balance circuits.”
5. The Brain Fog Recovery Breath
A neurological “reset” technique used in our NeuroRevive Program.
How to perform it:
- Sit upright
- Inhale sharply through the nose for 1 second
- Exhale slowly for 7–8 seconds
- Repeat 6 times
This improves cortical activation and clarity.
Image note: “Patient practicing a long exhale brain fog recovery breathing technique with a clinician guiding posture.”
How We Use Breathing in Clinical Treatment Plans
At California Brain & Spine Center, breathing exercises are integrated into advanced therapeutic programs such as:
- Vestibular Rehabilitation
- Cognitive Rehabilitation
- Neuroplasticity-based protocols
- Dysautonomia recovery programs
- NeuroSensory Integration (NSI)
- Low-Level Laser Therapy (LLLT)
- PEMF and GammaCore vagus nerve stimulation
- NeuroRevive brain rehabilitation program
Breathing enhances these treatments by stabilizing the autonomic system, improving oxygen efficiency, and reducing neurological noise.
“Breathing is the simplest therapy with the greatest neurological impact—when guided correctly.”
A Real Patient Story From My Clinic
A patient named Michael came to my clinic struggling with dizziness, anxiety spikes, and persistent brain fog following a mild concussion. He had been told repeatedly that his symptoms were “just stress,” but his instinct told him something deeper was happening.
During his evaluation, we identified autonomic imbalance affecting his vestibular system—something commonly missed in standard assessments.
We created a treatment plan that included:
- targeted vestibular rehab
- NeuroRevive cognitive work
- daily breathing protocols
Within weeks, Michael reported that his dizziness had decreased, his thinking felt clearer, and his confidence returned.
He told me:
“Breathing felt too simple at first, but it changed everything once I understood how it affects my brain.”
Stories like his are why I emphasize breathing as a core neurological tool—not an afterthought.
Your Most Common Questions About Breathing for Dizziness and Brain Fog
- Can breathing exercises stop dizziness immediately?
Sometimes yes—especially when dizziness is related to anxiety or CO2 imbalance. In other cases, breathing reduces symptoms gradually as the nervous system stabilizes. - Is dizziness from breathing dangerous?
Dizziness caused by hyperventilation is uncomfortable but generally not dangerous. However, persistent dizziness should always be evaluated. - Can breathing help with post-concussion brain fog?
Absolutely. Breathing influences brain perfusion, autonomic stability, and cognitive control—critical areas affected after concussion. - How often should I practice these exercises?
Most patients benefit from 2–3 sessions daily, each lasting 3–6 minutes. - Do I need a specialist to guide these techniques?
Guidance helps, especially if dizziness or brain fog is severe, but you can safely begin the exercises on your own.
Conclusion
Breathing exercises are one of the most powerful tools for calming dizziness, reducing anxiety, and clearing brain fog. They work by stabilizing the autonomic nervous system, improving brain oxygenation, and supporting balance processing.
As someone who evaluates dizziness and neurological imbalance daily, I’ve seen how transformative these techniques can be—especially when combined with a comprehensive treatment plan.
If you are experiencing persistent dizziness or brain fog, breathing exercises are a valuable starting point, but a proper neurological and vestibular evaluation can help identify the underlying causes.
Ready to Take the Next Step?
If you want personalized guidance or feel your symptoms need deeper evaluation, you are welcome to schedule a visit at California Brain & Spine Center in Calabasas. Together, we can build a care plan designed to restore clarity, confidence, and long-term stability.
Comments
FAQ
What is Functional Neurology?
Functional Neurology is a healthcare specialty that focuses on assessing and rehabilitating the nervous system’s function. It emphasizes neuroplasticity—the brain’s ability to adapt and reorganize—using non-invasive, evidence-based interventions to improve neurological performance.
How does Functional Neurology differ from traditional neurology?
Traditional neurology often concentrates on diagnosing and treating neurological diseases through medications or surgery. In contrast, Functional Neurology aims to optimize the nervous system’s function by identifying and addressing dysfunctions through personalized, non-pharmaceutical interventions.
Is Functional Neurology a replacement for traditional medical care?
No. Functional Neurology is intended to complement, not replace, traditional medical care. Practitioners often collaborate with medical professionals to provide comprehensive care.
What conditions can Functional Neurology help manage?
Functional Neurology has been applied to various conditions, including:
• Concussions and Post-Concussion Syndrome
• Traumatic Brain Injuries (TBI)
• Vestibular Disorders
• Migraines and Headaches
• Neurodevelopmental Disorders (e.g., ADHD, Autism)
• Movement Disorders
• Dysautonomia
• Peripheral Neuropathy
• Functional Neurological Disorder (FND)
Can Functional Neurology assist with neurodegenerative diseases?
While Functional Neurology does not cure neurodegenerative diseases, it can help manage symptoms and improve quality of life by optimizing the function of existing neural pathways.
What diagnostic methods are used in Functional Neurology?
Functional Neurologists employ various assessments, including:
• Videonystagmography (VNG)
• Computerized Posturography
• Oculomotor Testing
• Vestibular Function Tests
• Neurocognitive Evaluations
How is a patient’s progress monitored?
Progress is tracked through repeated assessments, patient-reported outcomes, and objective measures such as balance tests, eye movement tracking, and cognitive performance evaluations.
What therapies are commonly used in Functional Neurology?
Interventions may include:
- Vestibular Rehabilitation
- Oculomotor Exercises
- Sensorimotor Integration
- Cognitive Training
- Balance and Coordination Exercises
- Nutritional Counseling
- Lifestyle Modifications
Are these therapies personalized?
Absolutely. Treatment plans are tailored to the individual’s specific neurological findings, symptoms, and functional goals.
Who can benefit from Functional Neurology?
Individuals with unresolved neurological symptoms, those seeking non-pharmaceutical interventions, or patients aiming to optimize brain function can benefit from Functional Neurology.
Is Functional Neurology suitable for children?
Yes. Children with developmental delays, learning difficulties, or neurodevelopmental disorders may benefit from Functional Neurology approaches.
How does Functional Neurology complement other medical treatments?
It can serve as an adjunct to traditional medical care, enhancing outcomes by addressing functional aspects of the nervous system that may not be targeted by conventional treatments.
How is technology integrated into Functional Neurology?
Technological tools such as virtual reality, neurofeedback, and advanced diagnostic equipment are increasingly used to assess and enhance neurological function.
What is the role of research in Functional Neurology?
Ongoing research continues to refine assessment techniques, therapeutic interventions, and our understanding of neuroplasticity, contributing to the evolution of Functional Neurology practices.

Dr. Alireza Chizari
Latest articles