Headaches are common, but not all migraines look the same. Some people experience intense throbbing head pain, while others primarily suffer from dizziness, vertigo, and balance problems—sometimes without significant head pain at all. These symptoms often point to a condition known as vestibular migraine, which is frequently confused with a traditional migraine or even inner ear disorders.
Vestibular Migraine vs. Regular Migraine: Symptoms, Causes
I’m Dr. Alireza Chizari, neurologist at California Brain & Spine Center in Calabasas. Over the years, I’ve seen many patients who spent months—or even years—trying to understand why they felt constantly dizzy, off balance, or motion-sensitive. In many cases, the underlying cause was vestibular migraine, a condition that requires a slightly different diagnostic approach and treatment strategy than a classic migraine.
In this guide, I’ll explain how vestibular migraine differs from a regular migraine, the key symptoms that help distinguish them, and the most effective treatment approaches.
What Is a Regular Migraine?
A classic migraine (also called migraine without vestibular features) is a neurological condition characterized primarily by recurrent headaches with specific associated symptoms.
Typical migraine headaches often involve:
- Throbbing or pulsating pain, often on one side of the head
- Sensitivity to light and sound
- Nausea or vomiting
- Visual disturbances (aura) in some patients
- Pain that worsens with physical activity
Migraine attacks usually last 4 to 72 hours, and many patients experience recognizable triggers such as stress, sleep changes, dehydration, or hormonal fluctuations.
“Migraine is not simply a headache—it’s a complex neurological disorder involving changes in brain signaling, blood vessels, and sensory processing.”
What Is Vestibular Migraine?
Vestibular migraine is a subtype of migraine where dizziness and balance disturbances are the dominant symptoms.
Instead of severe head pain, patients may experience:
- Vertigo (spinning sensation)
- Chronic dizziness or imbalance
- Motion sensitivity
- Difficulty focusing vision during movement
- Light and sound sensitivity
Interestingly, some vestibular migraine episodes occur without any headache at all, which is why many people initially believe they have an inner ear problem rather than a neurological condition.
Key Differences Between Vestibular Migraine and Regular Migraine
While both conditions share a neurological origin, their primary symptoms and clinical presentation differ.
1. Dominant Symptoms
Regular Migraine
- Severe headache
- Pulsating pain
- Nausea and light sensitivity
Vestibular Migraine
- Vertigo or dizziness
- Balance instability
- Motion sensitivity
- Sometimes minimal or no head pain
2. Duration of Episodes
Vestibular migraine episodes can last:
- Minutes
- Hours
- Several days
Classic migraine headaches typically last 4–72 hours.
3. Sensory Triggers
Both types share triggers, but vestibular migraine is often triggered by:
- Busy visual environments
- Scrolling screens
- Motion (cars, elevators)
- Crowded spaces
4. Misdiagnosis
Vestibular migraine is frequently mistaken for:
- Benign Paroxysmal Positional Vertigo (BPPV)
- Ménière’s disease
- Chronic dizziness or anxiety-related dizziness
Correct diagnosis requires careful neurological and vestibular evaluation.
Why Vestibular Migraine Happens
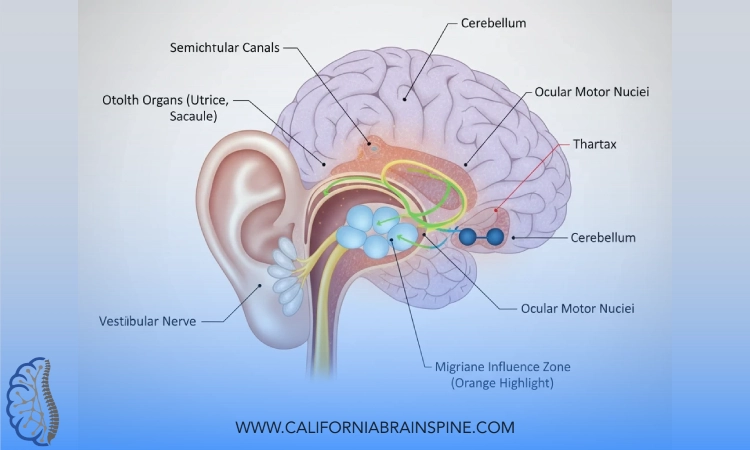
Vestibular migraine likely develops due to abnormal communication between migraine pathways and the brain’s balance centers.
These include:
- The vestibular nuclei in the brainstem
- The cerebellum, which controls coordination
- Sensory processing regions that integrate visual and balance signals
During a vestibular migraine attack, these systems become temporarily dysregulated, leading to dizziness, disorientation, and motion intolerance.
“Vestibular migraine represents an overlap between migraine biology and the brain’s balance network.”
Real Patient Story: When Dizziness Wasn’t an Inner Ear Problem
A patient in her early 40s came to our clinic after nearly a year of persistent dizziness. She had undergone multiple ENT evaluations and imaging studies that showed no structural abnormalities.
Her symptoms included:
- Sudden vertigo spells
- Sensitivity to bright lights
- Difficulty walking in busy environments
After a detailed neurological history and vestibular assessment, we identified the pattern of vestibular migraine. With targeted migraine prevention therapy and vestibular rehabilitation, her dizziness episodes decreased dramatically within a few months.
Treatment Approaches: How They Differ
Although both conditions share treatment strategies, vestibular migraine management often emphasizes balance-related rehabilitation in addition to migraine control.
Lifestyle and Trigger Management
Patients benefit from identifying and minimizing common migraine triggers:
- Sleep irregularities
- Dehydration
- Stress
- Caffeine fluctuations
- Hormonal changes
Preventive Medications
Depending on severity and frequency, neurologists may prescribe:
- Beta blockers
- Calcium channel blockers
- Anti-seizure medications
- CGRP-targeting therapies
These medications stabilize migraine pathways in the brain.
Vestibular Rehabilitation Therapy
For vestibular migraine patients experiencing persistent imbalance, vestibular therapy exercises can retrain the brain’s balance system and reduce motion sensitivity.
Stress and Nervous System Regulation
Stress management techniques such as:
- Breathing exercises
- Mindfulness training
- Gradual exposure to motion triggers
can significantly reduce attack frequency.
“Effective treatment often combines neurological care, lifestyle adjustments, and targeted vestibular rehabilitation.”
When to Seek Evaluation
If you experience recurrent dizziness, vertigo, or motion sensitivity—especially if accompanied by migraine symptoms—it’s important to seek specialized evaluation.
Consider consulting a neurologist if you have:
- Frequent dizziness episodes with or without headache
- Vertigo triggered by visual motion or busy environments
- Migraine history combined with balance problems
- Persistent symptoms that interfere with daily activities
At California Brain & Spine Center, we perform comprehensive neurological and vestibular assessments to determine whether symptoms stem from migraine, inner ear disorders, or other neurological causes.
Key Takeaways
- Vestibular migraine primarily causes dizziness and balance problems, while regular migraine mainly causes head pain.
- Vestibular migraine attacks may occur without headache, making diagnosis more challenging.
- Both conditions share neurological origins but may require different treatment strategies.
- Accurate diagnosis allows for targeted therapy that can significantly improve quality of life.
Frequently Asked Questions
- Can vestibular migraine occur without headaches?
Yes. Many patients experience vertigo or dizziness without significant head pain, which often leads to delayed diagnosis. - Is vestibular migraine an inner ear disorder?
No. It is primarily a neurological condition, although it affects the brain’s balance system. - How long do vestibular migraine episodes last?
Episodes may last from minutes to several days, depending on severity and triggers. - Can vestibular migraine be cured?
While there is no permanent cure, proper treatment and lifestyle management can greatly reduce attack frequency and severity.
Final Thoughts
When patients experience dizziness, vertigo, and migraine symptoms together, the underlying cause is not always obvious. Understanding the difference between vestibular migraine and traditional migraine is essential for proper treatment.
At California Brain & Spine Center, my goal is to help patients uncover the true source of their symptoms and create a treatment plan that restores stability, clarity, and confidence in everyday life.
If dizziness or migraine symptoms are affecting your daily activities, a comprehensive neurological evaluation may be the first step toward relief.
Comments
FAQ
What is Functional Neurology?
Functional Neurology is a healthcare specialty that focuses on assessing and rehabilitating the nervous system’s function. It emphasizes neuroplasticity—the brain’s ability to adapt and reorganize—using non-invasive, evidence-based interventions to improve neurological performance.
How does Functional Neurology differ from traditional neurology?
Traditional neurology often concentrates on diagnosing and treating neurological diseases through medications or surgery. In contrast, Functional Neurology aims to optimize the nervous system’s function by identifying and addressing dysfunctions through personalized, non-pharmaceutical interventions.
Is Functional Neurology a replacement for traditional medical care?
No. Functional Neurology is intended to complement, not replace, traditional medical care. Practitioners often collaborate with medical professionals to provide comprehensive care.
What conditions can Functional Neurology help manage?
Functional Neurology has been applied to various conditions, including:
• Concussions and Post-Concussion Syndrome
• Traumatic Brain Injuries (TBI)
• Vestibular Disorders
• Migraines and Headaches
• Neurodevelopmental Disorders (e.g., ADHD, Autism)
• Movement Disorders
• Dysautonomia
• Peripheral Neuropathy
• Functional Neurological Disorder (FND)
Can Functional Neurology assist with neurodegenerative diseases?
While Functional Neurology does not cure neurodegenerative diseases, it can help manage symptoms and improve quality of life by optimizing the function of existing neural pathways.
What diagnostic methods are used in Functional Neurology?
Functional Neurologists employ various assessments, including:
• Videonystagmography (VNG)
• Computerized Posturography
• Oculomotor Testing
• Vestibular Function Tests
• Neurocognitive Evaluations
How is a patient’s progress monitored?
Progress is tracked through repeated assessments, patient-reported outcomes, and objective measures such as balance tests, eye movement tracking, and cognitive performance evaluations.
What therapies are commonly used in Functional Neurology?
Interventions may include:
- Vestibular Rehabilitation
- Oculomotor Exercises
- Sensorimotor Integration
- Cognitive Training
- Balance and Coordination Exercises
- Nutritional Counseling
- Lifestyle Modifications
Are these therapies personalized?
Absolutely. Treatment plans are tailored to the individual’s specific neurological findings, symptoms, and functional goals.
Who can benefit from Functional Neurology?
Individuals with unresolved neurological symptoms, those seeking non-pharmaceutical interventions, or patients aiming to optimize brain function can benefit from Functional Neurology.
Is Functional Neurology suitable for children?
Yes. Children with developmental delays, learning difficulties, or neurodevelopmental disorders may benefit from Functional Neurology approaches.
How does Functional Neurology complement other medical treatments?
It can serve as an adjunct to traditional medical care, enhancing outcomes by addressing functional aspects of the nervous system that may not be targeted by conventional treatments.
How is technology integrated into Functional Neurology?
Technological tools such as virtual reality, neurofeedback, and advanced diagnostic equipment are increasingly used to assess and enhance neurological function.
What is the role of research in Functional Neurology?
Ongoing research continues to refine assessment techniques, therapeutic interventions, and our understanding of neuroplasticity, contributing to the evolution of Functional Neurology practices.

Dr. Alireza Chizari
Latest articles

