Dizziness following a concussion can be one of the most frustrating and persistent symptoms. Even months after the initial injury, many individuals continue to experience vertigo, imbalance, and disorientation. But why does this happen? Often, the culprit is hidden vestibular damage — subtle injuries to the inner ear and the vestibular system that are not always apparent on standard scans or examinations.
Why You Still Feel Dizzy Months After a Concussion?
I’m Dr. Alireza Chizari, a neurologist at California Brain & Spine Center in Calabasas, and my focus is on diagnosing and treating complex post-concussion symptoms, including persistent dizziness.
In this article, I will explain why dizziness can linger after a concussion, what hidden vestibular damage is, and how targeted treatment can restore your balance and quality of life.
The Connection Between Concussion and Vestibular Function
A concussion often involves a blow or jolt to the head that disrupts brain function temporarily. However, underneath the surface, it can also cause damage to the vestibular system — the sensory system responsible for balance, spatial orientation, and eye movements.
The vestibular system is composed of:
- The inner ear structures (semicircular canals and otolith organs)
- The vestibular nerve
- Central connections in the brainstem and cerebellum
If any part of this system sustains damage, it can lead to symptoms such as:
- Persistent dizziness or vertigo
- Imbalance or unsteady gait
- Visual disturbances with head movement
- Feelings of disorientation or motion sensitivity
Crucially, many of these injuries are microscopic and not visible on typical imaging scans, which is what we refer to as hidden vestibular damage.
“Concussions can injure the delicate sensors of your inner ear in ways that aren’t obvious on scans but cause ongoing dizziness and imbalance.”
Why Do Some People Feel Dizziness Months After a Concussion?
Some individuals recover quickly, but a significant number experience long-lasting vestibular symptoms. Several reasons explain this persistence:
1. Microstructural Inner Ear Damage
The delicate hair cells within the semicircular canals or otolith organs may be stretched, damaged, or dislodged, impairing the nerve signals that inform your brain about head position.
2. Vestibular Neuropathy
Damage to the vestibular nerve fibers can disrupt communication from the inner ear to the brain, leading to abnormal perception of movement and balance issues.
3. Central Vestibular Processing Issues
Even if peripheral structures are intact, the brainstem or cerebellum may have been affected, impairing the integration of sensory signals necessary for stability.
4. Co-existing Inner Ear Conditions
In some cases, pre-existing or concurrent inner ear disorders (like benign paroxysmal positional vertigo — BPPV) can be triggered or worsen after trauma.
5. Incomplete Symptom Resolution
The brain and ear may undergo gradual recovery at different rates. Residual microscopic injuries can cause persistent symptoms even when symptoms of a concussion seem to resolve.
Scientific insight: Studies show that even minor injuries to the vestibular apparatus can produce disabling dizziness—often underestimated by standard clinical exams.
How We Diagnose Hidden Vestibular Damage
Diagnosing subtle inner ear injuries requires specialized testing beyond basic physical exam:
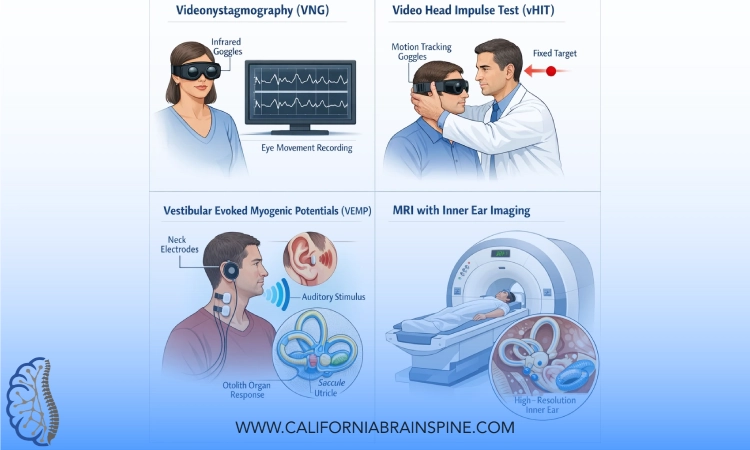
At California Brain & Spine Center, we utilize advanced diagnostics to uncover these hidden injuries, guiding targeted therapies.
Treatment Options for Persistent Vestibular Dysfunction
If hidden vestibular damage is confirmed, specific rehabilitative therapies can significantly improve symptoms:
1. Vestibular Rehabilitation Therapy (VRT)
A customized program of exercises designed to:
- Promote compensation and adaptation
- Reduce dizziness and imbalance
- Improve visual stability during head movement
2. Canalith Repositioning Maneuvers
For cases of BPPV, precise maneuvers like the Epley maneuver can dislodge displaced otoliths causing vertigo.
3. Medication
In some cases, short-term use of vestibular suppressants may be helpful, but they are generally used sparingly to avoid delaying adaptation.
4. Treatment of Underlying Inner Ear Conditions
Addressing conditions such as inflammation, infection, or otolith dislodgement is key to recovery.
5. Multidisciplinary Approach
Incorporating neurologists, vestibular therapists, and audiologists ensures comprehensive care tailored to your needs.
“Addressing hidden vestibular damage requires a precise diagnosis and targeted therapy. Restoring balance is possible, even months after injury.”
A Personal Case: Overcoming Persistent Vestibular Symptoms
One patient, a 35-year-old cyclist, experienced dizziness and unsteadiness for over six months after hitting his head during a race. Standard scans showed no visible damage. After detailed vestibular testing, we identified bilateral semicircular canal dysfunction due to microscopic hair cell injury. With specialized vestibular rehab and repositioning maneuvers, he regained his balance and returned to normal activity within just a few months.
Summary: Why Persistent Dizziness Happens After a Head Injury
- Concussions can cause microscopic injuries to the inner ear’s delicate structures—these injuries are often unseen on MRI.
- Hidden vestibular damage can lead to ongoing vertigo, imbalance, and disorientation long after initial recovery.
- Advanced testing and targeted treatment are essential to restore your vestibular function and quality of life.
When to Consult a Specialist
If you’ve been feeling dizzy, unsteady, or disoriented months after a concussion, don’t delay seeking expert evaluation. Persistent vestibular symptoms can be effectively treated with the right strategies, improving your stability, safety, and confidence.
Comments
FAQ
What is Functional Neurology?
Functional Neurology is a healthcare specialty that focuses on assessing and rehabilitating the nervous system’s function. It emphasizes neuroplasticity—the brain’s ability to adapt and reorganize—using non-invasive, evidence-based interventions to improve neurological performance.
How does Functional Neurology differ from traditional neurology?
Traditional neurology often concentrates on diagnosing and treating neurological diseases through medications or surgery. In contrast, Functional Neurology aims to optimize the nervous system’s function by identifying and addressing dysfunctions through personalized, non-pharmaceutical interventions.
Is Functional Neurology a replacement for traditional medical care?
No. Functional Neurology is intended to complement, not replace, traditional medical care. Practitioners often collaborate with medical professionals to provide comprehensive care.
What conditions can Functional Neurology help manage?
Functional Neurology has been applied to various conditions, including:
• Concussions and Post-Concussion Syndrome
• Traumatic Brain Injuries (TBI)
• Vestibular Disorders
• Migraines and Headaches
• Neurodevelopmental Disorders (e.g., ADHD, Autism)
• Movement Disorders
• Dysautonomia
• Peripheral Neuropathy
• Functional Neurological Disorder (FND)
Can Functional Neurology assist with neurodegenerative diseases?
While Functional Neurology does not cure neurodegenerative diseases, it can help manage symptoms and improve quality of life by optimizing the function of existing neural pathways.
What diagnostic methods are used in Functional Neurology?
Functional Neurologists employ various assessments, including:
• Videonystagmography (VNG)
• Computerized Posturography
• Oculomotor Testing
• Vestibular Function Tests
• Neurocognitive Evaluations
How is a patient’s progress monitored?
Progress is tracked through repeated assessments, patient-reported outcomes, and objective measures such as balance tests, eye movement tracking, and cognitive performance evaluations.
What therapies are commonly used in Functional Neurology?
Interventions may include:
- Vestibular Rehabilitation
- Oculomotor Exercises
- Sensorimotor Integration
- Cognitive Training
- Balance and Coordination Exercises
- Nutritional Counseling
- Lifestyle Modifications
Are these therapies personalized?
Absolutely. Treatment plans are tailored to the individual’s specific neurological findings, symptoms, and functional goals.
Who can benefit from Functional Neurology?
Individuals with unresolved neurological symptoms, those seeking non-pharmaceutical interventions, or patients aiming to optimize brain function can benefit from Functional Neurology.
Is Functional Neurology suitable for children?
Yes. Children with developmental delays, learning difficulties, or neurodevelopmental disorders may benefit from Functional Neurology approaches.
How does Functional Neurology complement other medical treatments?
It can serve as an adjunct to traditional medical care, enhancing outcomes by addressing functional aspects of the nervous system that may not be targeted by conventional treatments.
How is technology integrated into Functional Neurology?
Technological tools such as virtual reality, neurofeedback, and advanced diagnostic equipment are increasingly used to assess and enhance neurological function.
What is the role of research in Functional Neurology?
Ongoing research continues to refine assessment techniques, therapeutic interventions, and our understanding of neuroplasticity, contributing to the evolution of Functional Neurology practices.

Dr. Alireza Chizari
Latest articles

