If vertigo keeps interrupting your day, you already know how unfair it feels. One moment you are fine, and the next the room feels like it shifts, spins, or tilts. You might worry about driving, grocery shopping, working on a screen, or even rolling over in bed. That constant uncertainty can make you feel like your life is shrinking.
I, Dr. Alireza Chizari, wrote this article to help you understand vertigo triggers to avoid and what makes vertigo worse in real life. You are the hero of this story. You are the one trying to stay functional while your nervous system sends confusing balance signals. My job is to be your guide, help you identify patterns, rule out dangerous causes, and build a personalized plan that respects your safety and your goals.
This page will show you the most common vertigo triggers to avoid, why they trigger symptoms, and what a thorough evaluation looks like at California Brain and Spine Center in Calabasas, California. If you are ready for clearer answers and a calm plan, you will know how to use our neurological and vestibular services to get help.
What vertigo really is and why the trigger pattern matters
Vertigo is a sensation of motion when you are not actually moving, or a sensation that your surroundings are moving around you. Some people feel spinning. Others feel pulling, rocking, floating, or sudden imbalance. Vertigo is not a diagnosis by itself. It is a symptom, and the cause can involve the inner ear, the brain, the neck, or how these systems communicate.
This is why vertigo triggers to avoid are so important. Triggers are not random. They are clues. If vertigo gets worse when you roll in bed or look up, that suggests a different pattern than vertigo that gets worse in busy stores, on screens, or in crowds. When we identify your trigger pattern, we can choose the right evaluation and the right treatment.
In my clinic, I always remind patients of one key truth: your symptoms have logic, even if they feel chaotic right now. Our job is to find the logic.
Vertigo triggers to avoid that commonly make symptoms worse
When someone searches for vertigo triggers to avoid, they usually want a simple list. I will give you practical guidance, but I also want you to understand why these triggers matter so you can make smarter decisions, not fearful ones.
Here are common vertigo triggers to avoid, or at least manage carefully until you have a clear diagnosis:
• Sudden head position changes, especially looking up or bending down quickly
• Rolling in bed fast, especially turning toward one side
• Dehydration and skipping meals, which can destabilize the nervous system
• Poor sleep, which lowers the brain’s tolerance for sensory input
• Bright, flickering lights and heavy screen scrolling
• Alcohol and high caffeine in sensitive phases
• High stress states that change breathing and muscle tension
Important: avoiding a trigger forever is rarely the goal. The goal is to avoid unnecessary flare cycles until the driver is identified, then retrain safely.
You do not need more willpower. You need a map, a diagnosis, and a plan.
The bed test problem: why rolling over can be one of the biggest triggers
When vertigo is worse with turning in bed?
If your vertigo spikes when you roll over, sit up, or look upward, one possibility is benign paroxysmal positional vertigo, often called BPPV. BPPV happens when tiny crystals in the inner ear move into a place where they disturb motion sensing. The vertigo can be intense but brief. It often comes with nausea and a sense of spinning.
Why “pushing through” can backfire?
If you repeatedly trigger positional vertigo without proper guidance, you can end up in a cycle of fear and sensitivity. That does not mean you are fragile. It means your balance system is being provoked without resolution. A correct evaluation can identify whether BPPV is present and whether specific repositioning maneuvers are appropriate.
Screens, stores, and visual overload: a modern vertigo trigger many people miss
Visual motion sensitivity can mimic vertigo
Many people experience dizziness and unsteadiness from visual motion sensitivity. Large stores with long aisles, fast moving crowds, patterned floors, and fluorescent lighting can overload the brain’s processing systems. Phones and computers can do the same, especially with quick scrolling.
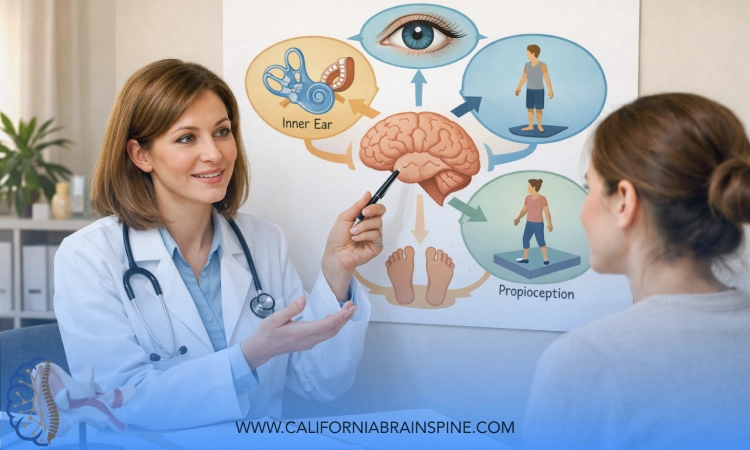
The brain and inner ear must agree
Your eyes, inner ears, and body position sensors must send matching information to your brain to create stability. When they do not match well, your brain may generate a motion sensation to explain the conflict. That can feel like vertigo, even if the inner ear is not the only driver.
Healing often starts when you stop asking “What is wrong with me?” and start asking “What is my system reacting to?”

What makes vertigo worse when the neck is involved?
Cervicogenic dizziness and neck driven imbalance
Some cases involve neck input that distorts balance signals. After a whiplash injury, a concussion, or prolonged neck tension, the sensors in the upper neck may send unclear information to the brain about head position. That mismatch can contribute to dizziness, unsteadiness, and in some cases a vertigo like sensation.
Why posture advice alone is not enough?
Generic posture tips rarely fix a true driver. If the neck is contributing, the evaluation must be precise. My Gonstead training taught me to be exact with biomechanics. My Clinical Neuroscience education taught me how strongly neck input can influence vestibular processing. When the neck is part of the problem, targeted care can change the entire symptom pattern.
How I evaluate vertigo triggers to avoid in a real clinical workup?
When you come to me in Calabasas with vertigo, I do not start with assumptions. I start with your story, your triggers, and a careful screening that respects safety.
A thorough evaluation often includes:
• Symptom pattern mapping, including timing, duration, and what makes it worse
• Balance and gait observation to see how the system stabilizes under load
• Eye movement screening and head movement tolerance testing
• Neck and upper spine assessment when history suggests involvement
• Screening questions that point toward migraine patterns, dysautonomia, or post concussion issues
I also pay attention to red flags. If your symptoms suggest a potentially serious neurological issue, you need urgent medical evaluation. My role is to guide you toward the right level of care, not to force every case into one box.
Image note: “A clinician guiding a patient through a gentle balance assessment in a modern clinic, safety focused posture, no text.”
When vertigo is a warning sign and you should not wait?
Not all vertigo is dangerous, but some symptoms require prompt care. Seek urgent medical evaluation if you have vertigo along with any of the following:
• New weakness in the face, arm, or leg
• New trouble speaking, swallowing, or seeing clearly
• Severe sudden headache unlike your usual
• Fainting, chest pain, or severe shortness of breath
• New numbness, confusion, or inability to walk safely
Your safety is not overreacting. It is wisdom.
Middle of the article: how care is approached at California Brain and Spine Center
At California Brain and Spine Center, patients are evaluated with a combination of neurological and vestibular focused screening, functional observation, and a careful look at how the body stabilizes movement. The clinic serves Calabasas and surrounding areas across Southern California, and many patients arrive after weeks or months of being told their tests look normal while their daily life feels unstable.
Care is planned based on the most likely driver and the patient’s tolerance. Vestibular Rehabilitation can be used when the balance system needs retraining, including gaze stability, habituation exercises, and balance integration. Cognitive Rehabilitation can be relevant when attention, brain fog, or processing speed issues accompany dizziness. Neuroplasticity Rehabilitation may support structured adaptation when the nervous system has become overly reactive. NeuroSensory Integration can be used to improve how visual, vestibular, and proprioceptive input are blended.
In select cases, supportive non invasive options may be considered as part of a personalized plan. These may include LLLT, PEMF, HBOT, GammaCore Vagus Nerve Stimulation, and the NeuroRevive Program. These are not used as generic add ons. They are chosen when clinically appropriate and integrated with the overall strategy for stability and function.
Why avoiding vertigo triggers is helpful, but avoiding life is not the goal
Vertigo triggers to avoid can protect you from repeated flare cycles, especially early on. But long term avoidance can make your world smaller and sometimes increase sensitivity. The right approach is strategic.
Strategic means:
• Reduce unnecessary provocation while diagnosis is unclear
• Build a plan to reintroduce normal movement safely when appropriate
• Train the system that is underperforming, rather than blaming the whole body
• Track progress in real life outcomes, not only symptom fear
The goal is not a perfect day. The goal is a bigger life with more confidence.
Image note: “A patient walking outdoors on a calm path with stable posture and relaxed expression, Southern California vibe, no text.”
A practical guide to vertigo triggers to avoid during the next seven days
If your vertigo is active right now, here is a safe way to think about the next week. This is not a substitute for medical advice, but it can help reduce unnecessary flares while you seek proper care.
Use this approach:
• Choose slower head movements, especially when bending or looking up
• Sit before you stand if you feel off, then pause and breathe
• Hydrate consistently and eat regular meals to stabilize your system
• Reduce fast screen scrolling temporarily, then reintroduce in short blocks
• Avoid alcohol while symptoms are active
• Protect sleep as a treatment tool, not a luxury
• If a specific bed turn triggers vertigo, move slowly and consider sleeping with extra head support until evaluated
If you are falling, vomiting repeatedly, or cannot walk safely, seek urgent care.
A short patient story before the conclusion
Some time ago, a patient named M. came to see me after a sudden episode of vertigo that began when turning in bed. M. started avoiding sleep positions, stopped driving, and felt anxious in stores because the dizziness would spike without warning. The biggest fear was not knowing what made it worse.
I began by mapping the vertigo triggers to avoid and identifying the pattern. We found that M. had a strong positional trigger, plus significant neck tension from months of guarding. We coordinated the plan around safety and tolerability. We used a structured approach that included Vestibular Rehabilitation strategies and gentle neuro sensory work to reduce reactivity, alongside precise evaluation of mechanical contributors. When appropriate, parts of a broader recovery strategy such as Neuroplasticity Rehabilitation and a structured program like the NeuroRevive Program can help organize care into clear steps.
Over time, M. reported fewer sudden spins, better tolerance when rolling in bed, and a return to driving short distances without fear. What mattered most was that M. felt in control again. That is what a good plan does.
Your most common questions about vertigo triggers to avoid
- What are the most common vertigo triggers to avoid at home
The most common vertigo triggers to avoid include sudden head position changes, rolling in bed quickly, dehydration, poor sleep, alcohol during active phases, and heavy screen scrolling. Your personal triggers may point to the underlying cause. - Does BPPV cause vertigo when rolling over in bed
Yes, BPPV commonly causes short intense vertigo episodes when turning in bed, looking up, or bending down. A proper evaluation can confirm this and guide safe repositioning maneuvers when appropriate. - Can anxiety make vertigo worse
Anxiety can amplify symptoms by changing breathing, muscle tension, and nervous system arousal. That does not mean vertigo is psychological. It means the nervous system state can increase sensitivity. A good plan addresses both the driver and the body’s stress response. - Why do screens and stores make my vertigo worse
Busy environments and screens can trigger visual motion sensitivity. When the brain struggles to integrate visual and vestibular signals, dizziness or a vertigo like sensation can worsen. This pattern is common after concussion and in migraine physiology. - When should I worry that vertigo is something serious
Seek urgent care if vertigo occurs with new weakness, trouble speaking, severe sudden headache, fainting, chest pain, confusion, or inability to walk safely. Safety comes first. - What kind of treatment can help beyond avoiding triggers
Treatment depends on the cause. Many patients benefit from Vestibular Rehabilitation, evaluation of neck contributors, and a personalized neurological approach. In select cases, supportive non invasive therapies may be considered as part of a structured plan.
Conclusion
I, Dr. Alireza Chizari, want you to leave this page with clarity. Vertigo triggers to avoid are not just a list. They are clues that help us understand whether your symptoms are positional, visual, neck related, migraine related, post concussion related, or connected to broader nervous system regulation. What makes vertigo worse is often predictable once we map the pattern carefully.
If you are dealing with vertigo in Calabasas or anywhere in Southern California, my team and I at California Brain and Spine Center can guide you through a thoughtful evaluation and a personalized plan that focuses on safety, function, and real life outcomes. You deserve more than generic advice. You deserve a path that makes sense.
If you are ready, contact California Brain and Spine Center to request an appointment or reach out for a personalized neurological and vestibular evaluation. Our goal is to help you move toward the best version of your life and function, not just manage isolated symptoms.
Comments
FAQ
What is Functional Neurology?
Functional Neurology is a healthcare specialty that focuses on assessing and rehabilitating the nervous system’s function. It emphasizes neuroplasticity—the brain’s ability to adapt and reorganize—using non-invasive, evidence-based interventions to improve neurological performance.
How does Functional Neurology differ from traditional neurology?
Traditional neurology often concentrates on diagnosing and treating neurological diseases through medications or surgery. In contrast, Functional Neurology aims to optimize the nervous system’s function by identifying and addressing dysfunctions through personalized, non-pharmaceutical interventions.
Is Functional Neurology a replacement for traditional medical care?
No. Functional Neurology is intended to complement, not replace, traditional medical care. Practitioners often collaborate with medical professionals to provide comprehensive care.
What conditions can Functional Neurology help manage?
Functional Neurology has been applied to various conditions, including:
• Concussions and Post-Concussion Syndrome
• Traumatic Brain Injuries (TBI)
• Vestibular Disorders
• Migraines and Headaches
• Neurodevelopmental Disorders (e.g., ADHD, Autism)
• Movement Disorders
• Dysautonomia
• Peripheral Neuropathy
• Functional Neurological Disorder (FND)
Can Functional Neurology assist with neurodegenerative diseases?
While Functional Neurology does not cure neurodegenerative diseases, it can help manage symptoms and improve quality of life by optimizing the function of existing neural pathways.
What diagnostic methods are used in Functional Neurology?
Functional Neurologists employ various assessments, including:
• Videonystagmography (VNG)
• Computerized Posturography
• Oculomotor Testing
• Vestibular Function Tests
• Neurocognitive Evaluations
How is a patient’s progress monitored?
Progress is tracked through repeated assessments, patient-reported outcomes, and objective measures such as balance tests, eye movement tracking, and cognitive performance evaluations.
What therapies are commonly used in Functional Neurology?
Interventions may include:
- Vestibular Rehabilitation
- Oculomotor Exercises
- Sensorimotor Integration
- Cognitive Training
- Balance and Coordination Exercises
- Nutritional Counseling
- Lifestyle Modifications
Are these therapies personalized?
Absolutely. Treatment plans are tailored to the individual’s specific neurological findings, symptoms, and functional goals.
Who can benefit from Functional Neurology?
Individuals with unresolved neurological symptoms, those seeking non-pharmaceutical interventions, or patients aiming to optimize brain function can benefit from Functional Neurology.
Is Functional Neurology suitable for children?
Yes. Children with developmental delays, learning difficulties, or neurodevelopmental disorders may benefit from Functional Neurology approaches.
How does Functional Neurology complement other medical treatments?
It can serve as an adjunct to traditional medical care, enhancing outcomes by addressing functional aspects of the nervous system that may not be targeted by conventional treatments.
How is technology integrated into Functional Neurology?
Technological tools such as virtual reality, neurofeedback, and advanced diagnostic equipment are increasingly used to assess and enhance neurological function.
What is the role of research in Functional Neurology?
Ongoing research continues to refine assessment techniques, therapeutic interventions, and our understanding of neuroplasticity, contributing to the evolution of Functional Neurology practices.

Dr. Alireza Chizari
Latest articles

